Why Stress Hormones Don't Reset After Poor Sleep
Apr 20, 2026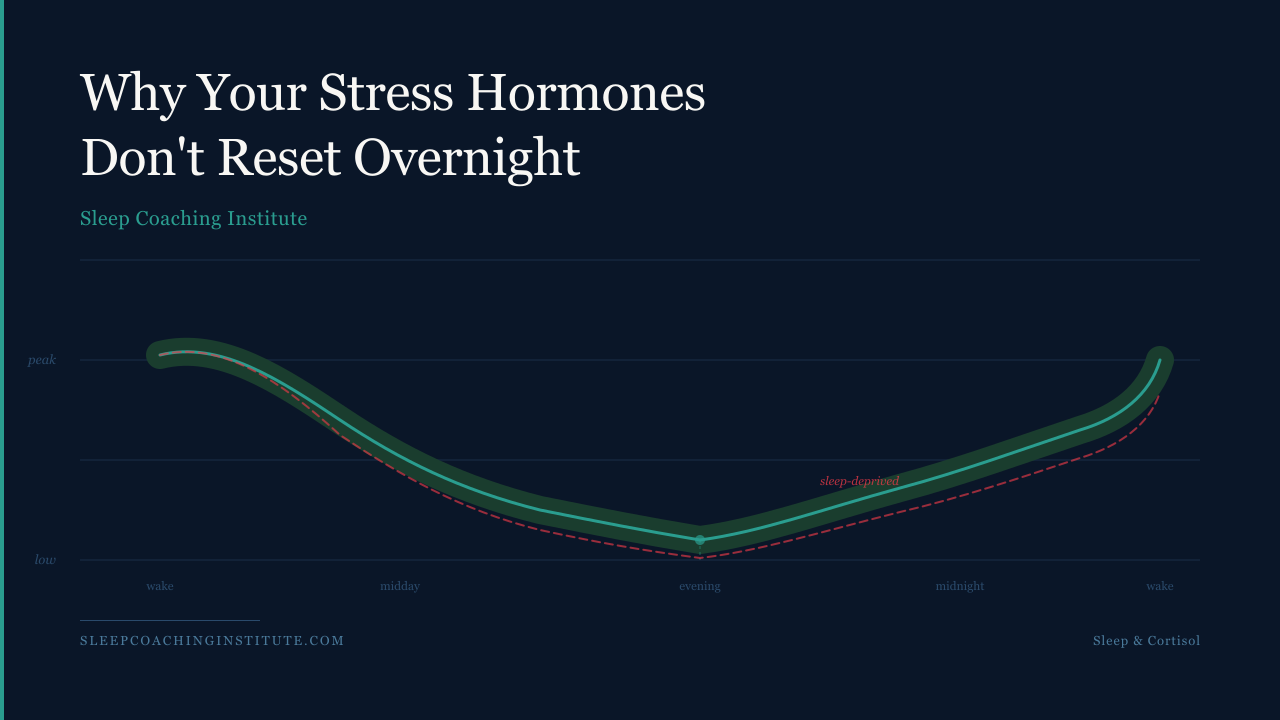
Key Findings
The HPA axis and sleep share a bidirectional relationship: sleep dampens HPA activity, but poor sleep elevates cortisol, which in turn disrupts the next night's sleep, creating a self-reinforcing cycle. (Nollet et al., 2020)
Interventional studies conducted in controlled laboratory environments show an increase in late afternoon and early evening cortisol with sleep loss, representing a flattening of the diurnal cortisol slope that is linked to mental and physical disease processes. (Czeisler et al., 2024)
Sleep deprivation amplifies cortisol reactivity to ordinary stressors, meaning sleep-deprived individuals produce a stronger hormonal stress response to the same inputs than rested individuals. (Nollet et al., 2020)
There is a particular kind of tired that does not feel like ordinary fatigue. You have slept, at least technically. You were in bed for seven or eight hours. But you wake up already braced, already running slightly hot, as if your body never fully stood down from the previous day. Your patience is shorter than it should be. Small frustrations feel disproportionate. You are tired but you cannot fully rest, which makes no sense until you understand what sleep deprivation actually does to the hormonal systems that are supposed to reset overnight.
The short version is that they do not reset. Not fully, and not quickly.
Cortisol, the body's primary stress hormone, follows a precise 24-hour rhythm under normal conditions. It peaks sharply in the early morning, within 30 to 45 minutes of waking, then declines gradually through the day, reaching its lowest point in the late evening. That evening trough is not incidental. It is the hormonal precondition for sleep. When cortisol drops low enough, the inhibitory pressure on the sleep system eases and the body can shift into genuine recovery. Disrupt the trough and you disrupt the entry point into restorative sleep. Poor sleep disrupts the trough. Which produces worse sleep. Which disrupts the trough again. The cycle is not a metaphor. It is a documented physiological feedback loop (Nollet et al., 2020).
The system responsible for cortisol production is called the HPA axis, short for hypothalamic-pituitary-adrenal. It functions like a chain of command. The hypothalamus detects a stressor, real or perceived, and signals the pituitary gland, which in turn signals the adrenal glands to release cortisol. Under normal conditions this chain activates, does its job, and then quiets down. Sleep is one of the primary mechanisms through which it quiets. Slow-wave sleep in particular suppresses HPA activity, giving the axis a recovery window it needs to respond appropriately the next day. When that sleep is shortened or fragmented, the suppression does not occur fully. The axis starts the next day already primed, already more reactive than it should be (Nollet et al., 2020).
What this looks like in practice is a flattening of the cortisol curve. The morning peak may remain but the evening decline becomes shallower and later. Instead of cortisol reaching its nadir by 10 or 11 pm, it stays elevated into the hours when the body is supposed to be winding down. Research using controlled laboratory sleep restriction protocols has confirmed this pattern repeatedly. Interventional studies show that sleep loss produces a measurable increase in late afternoon and early evening cortisol, a change that resembles the cortisol profiles associated with aging, chronic stress, and metabolic disease (Czeisler et al., 2024). The body is not failing. It is responding logically to a signal that says something is wrong. The problem is that the signal is being generated by the sleep deprivation itself.
The amplification effect compounds this further. Sleep-deprived individuals do not just have higher baseline cortisol. They produce a larger cortisol response to ordinary stressors than rested individuals do. The same meeting, the same difficult conversation, the same minor logistical frustration triggers a bigger hormonal reaction when sleep has been insufficient. This is not a weakness or a character trait. It is a calibration problem. The system that is supposed to modulate the stress response is running without its normal recovery window, and so it responds as if threats are larger than they are (Nollet et al., 2020).
The relationship also runs the other direction. Elevated cortisol in the evening actively interferes with sleep initiation. Cortisol is an alerting hormone. Its job, in the morning, is to mobilize glucose, increase heart rate, and prepare the body for the demands of the day. In the evening, those same effects work directly against the physiological conditions required for sleep onset. An elevated cortisol trough means the brain stays more alert than it should, sleep latency increases, and the slow-wave stages that would suppress HPA activity the following night are entered later and spent less time in. The cycle tightens (Nollet et al., 2020).
What makes this pattern particularly resistant to simple interventions is that it does not resolve with a single good night of sleep. Research on sleep recovery suggests that some aspects of HPA axis function normalize relatively quickly after sleep extension, but the behavioral and cognitive effects of accumulated sleep debt recover more slowly, and the hormonal sensitivity built up over days of poor sleep does not simply reset after one night (Czeisler et al., 2024). This is why people who finally get a full night of sleep after a difficult week often report feeling better but not fully restored. The axis needs more than one cycle to recalibrate.
Understanding this loop changes what practical sleep support looks like. The goal is not simply to get more hours. It is to create the conditions under which the HPA axis can complete its suppression cycle reliably. That means consistent sleep timing so the cortisol rhythm has an anchor point, light management in the evening so melatonin can rise without cortisol competition, and a genuine decompression window before bed rather than stimulating activity that keeps the axis active into the wind-down period.
For more on how circadian rhythm management connects to cortisol regulation, SCI's resources for professionals provide evidence-based frameworks for applying this in client work. The individual application of these principles is also covered in depth at SCI's resources for individuals, where the focus is on practical implementation rather than clinical theory.
The mechanisms described here look different depending on whether you are applying them in a professional context or to your own sleep. Both perspectives are worth addressing directly.
For Professionals
What This Means for Health and Wellness Professionals
Clients who present with perceived hyperreactivity, emotional dysregulation, or difficulty initiating sleep despite physical fatigue are frequently describing a neuroendocrine pattern rather than a behavioral or psychological one. The cortisol-sleep feedback loop is a clinical picture worth holding alongside the presenting complaint, not as a replacement for behavioral assessment but as a physiological frame that can change what interventions make sense.
The key clinical implication is that stress management and sleep improvement are not sequential. They are concurrent. A client working only on stress reduction without addressing sleep architecture is working against the underlying physiology. The HPA axis needs the suppression window that slow-wave sleep provides. Without that window, cortisol reactivity stays elevated regardless of how many other stress reduction techniques are applied. Intervening on sleep timing, light exposure, and evening arousal management alongside any stress-focused work is more likely to produce durable change than addressing either in isolation.
For client education, the feedback loop framing tends to be useful. Most people understand that stress causes poor sleep. Fewer understand that poor sleep causes a measurable increase in stress hormone output and amplifies their response to ordinary stressors. That bidirectional understanding shifts the conversation from willpower and habits to physiology, which tends to reduce shame and increase engagement with sleep-specific interventions.
Assessment questions worth incorporating: Does the client wake earlier than intended and struggle to return to sleep, which may indicate elevated early-morning cortisol? Do they describe feeling wired in the evening despite fatigue? Is sleep timing inconsistent, removing the anchor point the cortisol rhythm depends on? These patterns point toward HPA dysregulation as a contributing factor and help target interventions appropriately.
For professionals who want to build a structured clinical framework for assessing the sleep-stress-cortisol relationship and translating it into effective client protocols, the Certified Sleep Coach (CSC) program covers these mechanisms across five modules at $999 one-time or $189 per month for six months, carrying 0.6 continuing education units approved by NASM and AFAA.
For Individuals
How to Use This for Your Own Sleep
If you recognize the pattern described in this article, the wired-but-tired feeling, the disproportionate frustration, the sleep that does not fully restore, the most important thing to understand is that this is not a character flaw or a stress tolerance problem. It is a feedback loop with a specific physiological mechanism, and that means it can be interrupted with specific interventions.
The most effective single intervention for resetting a dysregulated cortisol rhythm is consistent wake time. Cortisol has a morning peak that is partly anchored to your habitual wake time. When that anchor is consistent, the whole rhythm becomes more predictable, the evening trough arrives more reliably, and the conditions for sleep onset improve. Varying your wake time by more than an hour, including on weekends, destabilizes the anchor and flattens the curve in the same direction as sleep deprivation does.
Evening light management matters more than most people realize. Cortisol and melatonin have an inverse relationship. Bright light in the evening, particularly from screens, suppresses melatonin and keeps cortisol from declining at its natural rate. Dimming your environment in the 60 to 90 minutes before bed is not a minor preference. It is a direct intervention on the hormonal conditions required for sleep onset.
A genuine decompression buffer matters for the same reason. Stimulating cognitive or emotional activity, work email, difficult conversations, engaging media, keeps the HPA axis active. A buffer of genuinely low-demand activity allows the axis to begin its evening descent. That descent is the door to restorative sleep.
If you want a structured approach to rebuilding your sleep rhythm from the ground up, The CORE System covers circadian reset, nervous system regulation, sleep drive, and environment across four modules with lifetime access, at $199 one-time.
Citations
Czeisler, C. A., Buxton, O. M., & Khalsa, S. B. S. (2024). Rhythms in cortisol mediate sleep and circadian impacts on health. Journal of Biological Rhythms. https://pmc.ncbi.nlm.nih.gov/articles/PMC11381560/
Leproult, R., Copinschi, G., Buxton, O., & Van Cauter, E. (1997). Sleep loss results in an elevation of cortisol levels the next evening. Sleep, 20(10), 865–870. https://doi.org/10.1093/sleep/20.10.865
National Institutes of Health. (2024). Brain basics: Understanding sleep. National Institute of Neurological Disorders and Stroke. https://www.ninds.nih.gov/health-information/public-education/brain-basics/brain-basics-understanding-sleep
Nollet, M., Wisden, W., & Franks, N. P. (2020). Sleep deprivation and stress: A reciprocal relationship. Interface Focus, 10(3), 20190092. https://doi.org/10.1098/rsfs.2019.0092
Spiegel, K., Leproult, R., & Van Cauter, E. (1999). Impact of sleep debt on metabolic and endocrine function. The Lancet, 354(9188), 1435–1439. https://doi.org/10.1016/S0140-6736(99)01376-8
Sleep affects everything. If you found this article useful, you will find even more inside the SCI library, including practical tools for professionals and individuals navigating real sleep challenges.
Stay connected with news and updates!
The science of sleep keeps moving. So do we. Join the SCI newsletter for evidence-based insights, new research, and practical tools delivered directly to the people who need them most.
Your information is never shared. Unsubscribe anytime